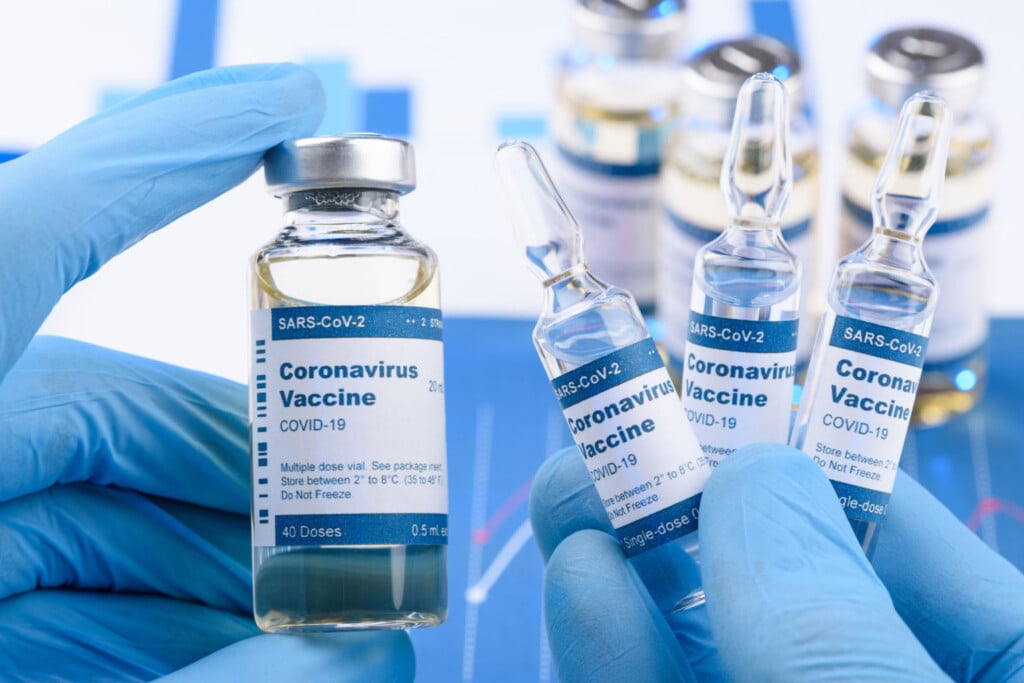
Drugmaker Pfizer announced this week that its COVID-19 vaccine was more than 90% effective as it shared preliminary data from a late-stage clinical trial.
It was welcome news in the midst of growing concerns about the coronavirus pandemic, which has sickened more than 50 million people and killed over a million worldwide — including nearly 250,000 in the United States. Anthony Fauci, director of the National Institute of Allergy and Infectious Diseases, called the results “extraordinary.”
If Pfizer receives authorization from the Food and Drug Administration for its vaccine, as is widely expected, it could potentially begin vaccinating millions of Americans before the end of the year.
USC experts discuss the company’s — and its competitors’ — vaccine technologies, potential regulatory hurdles and when a vaccine may be available to the public.
Ethical issues could complicate development of other vaccines
“While the data details are not clear at this time, there is no way not to celebrate this as a monumental achievement and a great first step forward towards controlling this devastating pandemic,” said Edward Jones-López, an infectious disease expert at the Keck School of Medicine of USC and investigator of an Operation Warp Speed vaccine clinical trial. “If the 90% efficacy estimate is corroborated, the efficacy of this vaccine will be among the highest when compared to other very successful vaccines.”
However, potential challenges remain.
“The trickiest issue is to determine how the Pfizer vaccine — and other front-runner candidates such as Moderna — results will affect the ethical and scientific integrity of the other ongoing vaccine studies,” he said.
Those vaccines are likely to be approved under an emergency use authorization, which by definition is based on preliminary or incomplete data. For that reason, as well as the fact that more than one vaccine will be needed to address the worldwide emergency, it’s important that other vaccine studies continue, Jones-López said.
Yet the approval of a vaccine, even under emergency use standards, is likely to disturb the equipoise — or balance of interests — that allows researchers to compare other vaccine candidates to a placebo.
“This tension, which is very unique to this moment, is likely to complicate several of the ongoing studies and potentially threaten their scientific and ethical integrity,” he warned. “Despite this, there’s an obvious need to develop more vaccines to address the global need.”
Pfizer announcement comes as infections increase
“Ironically, Pfizer was able to announce its results earlier than expected because of how out of control the pandemic has become,” said Steven Fox, an assistant research professor in the Department of Pharmaceutical and Health Economics at the USC School of Pharmacy and a fellow at the USC Schaeffer Center for Health Policy & Economics.
“With more than 100,000 new cases per day just in the U.S., the trial observed many more positive cases in the control arm, more quickly than expected,” he explained. “So in a way, it was the ineffectiveness of national pandemic control efforts that helped to rush the vaccine’s development.”
Fox listed the remaining issues to work out, including confirming safety for a full two months, monitoring long-term safety and efficacy, clarifying efficacy by risk group, ramping up production, prioritizing distribution and overcoming logistical distribution challenges.
“Nevertheless, with this news, we appear to be either at the end of the beginning or possibly even at the beginning of the end of the pandemic,” he said.
Pfizer COVID-19 vaccine uses genetic material
“The Pfizer vaccine is based on RNA, small snips of genetic material with the instructions to make coronavirus spike proteins once injected into a body,” said Paula Cannon, Distinguished Professor of Molecular Microbiology & Immunology at the Keck School of Medicine. “But RNA is very unstable, and the vaccine needs to be at extremely low temperatures all the time.”
Cannon explained that this creates a problem for transportation as well as storage in a pharmacy or doctor’s office, meaning the initial rollout could be limited to large centers with temperature-control capabilities.
“Hoped-for advances in the chemistry of RNA may provide a version in the future that is stable under less extreme temperatures,” she added.
What happens next?
Pfizer will likely seek an emergency use authorization from the FDA based on the results of the interim analysis, said Eunjoo Pacifici, an associate professor and chair of the Department of Regulatory and Quality Sciences at the USC School of Pharmacy.
“The FDA has provided the industry with clear guidance outlining the requirements for safety and effectiveness before a vaccine is authorized for emergency use,” Pacifici said. She explained that obtaining the emergency authorization doesn’t indicate that the product has full marketing approval: “It is important to keep in mind that the only way to ensure long-term safety and efficacy of a product is to assess safety and efficacy long term.”
Soeren Mattke, director of the Center for Improving Chronic Illness Care at the USC Dornsife College of Letters, Arts and Sciences, sounded a similar note of caution.
“The science is fascinating, but there has not yet been a single product approved using this technology and we are injecting genetic material into patients,” he warned. “Granted, messenger RNA is short-lived and won’t get integrated into your genome. Still, we would normally not ‘pilot’ such a novel technology in literally billions of patients, and unexpected things that you would theoretically not expect do happen.”
Pfizer’s COVID-19 vaccine was a ‘high risk, high reward effort’
Unlike other drug companies contracting with the United States under Operation Warp Speed for the development of a COVID-19 vaccine, Pfizer — and its German partner BioNTech — chose not to accept federal money for research and development. That decision paid off, said Shon Hiatt, an associate professor at the USC Marshall School of Business who researches entrepreneurship, strategy, regulatory affairs and business sustainability.
“This has freed the company from bureaucratic red tape during its phase 1-3 trials that could have slowed the process, and it also reduces the potential for future litigation against ownership issues and application of [intellectual property] developed from the vaccine,” said Hiatt, who noted that Pfizer got a $1.95 billion deal with the U.S. government under Operation Warp Speed to distribute 100 million doses and can negotiate a contract for another 500 million.
“So far, Pfizer has invested over $1.5 billion in the development of the vaccine. This was a high-risk, high-reward effort with an extremely quick drug development time period. If the high efficacy stands, this could be a financial win for Pfizer and even a greater reputational win for the company,” he predicted.
The partisan divide on requiring a COVID-19 vaccine
“For any vaccine to work on a large scale, the government and the people will have to be willing and ready to take the vaccine,” said Christian Grose, a USC Dornsife associate professor of political science and public policy and academic director of the USC Schwarzenegger Institute for State and Global Policy.
“In responding to a new USC Schwarzenegger Institute poll, a majority of voters supported a law that would require that a COVID-19 vaccine be given to all California residents. But there is a significant partisan divide, which is troubling from a public health standpoint. This suggests we will need not only a vaccine but a significant bipartisan messaging campaign about the importance of a vaccine.”